Jump to content
Glaucoma
Glaucoma is a condition that occurs when there is increased pressure within the eye. The normal eye pressure is 10-25mmHg, when the pressure is >30mmHg a diagnosis of glaucoma is made. If left untreated this condition can rapidly lead to blindness and become extremely painful. As it progresses there may be stretching and enlargement of the eye.
Causes
Primary Glaucoma
This is a hereditary condition where the normal angle of fluid drainage within the eye is too narrow and becomes blocked. It is seen in breeds such as the Shih Tzu, Jack Russell Terrier, Australian Cattle Dog, Basset Hound, Cocker Spaniel and Siberian husky. It usually begins in one eye and eventually presents in the second eye. It is very rare to see this condition in cats.
Secondary Glaucoma
This is the result of a disease or injury that has affected the eye and interrupts the drainage of aqueous fluid. Some of the diseases that can cause secondary glaucoma include severe cataracts, cancer of the eye, lens dislocation and ocular inflammation (uveitis).
Symptoms
- Vision loss
- Dilated pupil
- Redness in the white part of the eye
- Bulging eye
- Squinting or blinking of the eye
- Loss of appetite
- Headaches (head pressing due to pain)
Diagnosis
Unfortunately by the time you identify a problem and your vet has diagnosed your pet with glaucoma vision may have already been lost. Early intervention is the key! It can be prudent to regularly monitor eye pressure of at risk breeds at their annual health check. In some cases pet owners will have no idea that their pet is suffering from a degree of vision loss.
To diagnose glaucoma your vet will need a thorough history, especially any details of possible accidents involving an eye injury. The vet will use a tonometer to measure the pressure in each eye. In some cases your vet may need to refer your pet to an ophthalmologist.
Treatment
If your pet is diagnosed with glaucoma your vet will prescribe the appropriate treatments to lower the pressure in the eye/s and provide pain relief. If vision is saved, you may consider referral to a specialist ophthalmologist who can laser treat the abnormal drainage angle in the eye. In severe cases where the pressure and pain cannot be controlled medically, the best-case scenario may be to remove the eye itself with surgery.
If you suspect your dog may have glaucoma or is suffering from any of the above symptoms please book in for an appointment with your veterinarian.

Cataracts
What are cataracts?
A cataract is opacity within the lens of the eye and is one of the most common causes of blindness in pets. It may look like a white shading or fogginess over the eye. The opacity can be very small and not affect vision however cataracts will progress and in due time cause blindness.
How are cataracts caused?
Cataracts are mostly inherited with an early onset. Other factors like disease, trauma and old age may also contribute. In some cases pets can be born with cataracts as a result of toxins and infection during pregnancy. Cataracts can also be commonly associated with diabetes.
Diagnosis
Cataracts are generally easily diagnosed. Your veterinarian will discuss your pet’s health, onset and nature of the symptoms. In some cases diagnostic tests are performed to assist with the diagnosis, these can include, a complete blood count, biochemistry and urine analysis.
Treatment
Unfortunately medications are not successful in treating cataracts. Surgery is the only cure, although it is not always warranted as it depends of the degree of blindness and age. If your pet requires cataract surgery we would need to refer you to a specialist.
Conjunctivitis
What is it?
The conjunctiva is the mucous membrane that covers the white part of the eye and the inside of the eyelids. Conjunctivitis is inflammation of the conjunctiva. Conjunctivitis has many causes, some contagious and others not. Unlike in humans, where most cases are bacterial, conjunctivitis in dogs is often allergic in nature and in cats is typically due to chronic viral infections (such as Herpesvirus).
Causes
- Pollens or allergies
- Dust or windy conditions (particularly in dogs with prominent eyes such as Pugs, Shih Tzu’s or Pekingnese)
- Dry Eye (inadequate tear production)
- Irritants such as perfumes and incense
- Injury to the eye (e.g. rubbing, foreign body)
- Entropian, where the eyelid rolls inward and hairs rub the eye
- Infectious (bacterial or viral) Is it contagious to humans? Generally no. However, rare cases of Chlamydia infections in cats can be, so it is important to wash your hands after handling.
Diagnosis
Diagnosis of conjunctivitis can be made on examination by your veterinarian. Other diagnostic tests may be needed to determine the underlying cause such as cytology of the discharge, Schirmer Tear Test to measure tear production, or a swab for certain viral diseases (particularly in cats). A fluoroscein dye can be used to determine if there is a scratch or ulcer present. The stain adheres to injured cornea and ‘glows’ green under UV light, that way your vet will easily be able to identify an injury. This examination is not painful for your pet. What if there is a scratch or ulcer? See Corneal Ulcer Blog (there will be a link here)
Treatment
Depending on the cause of conjunctivitis, different treatments may be recommended, such as:
- Topical and/or oral antibiotics
- Antihistamines
- Steroids
- Eye lubricants, and/or medications to increase tear production
- Surgery to correct eyelid abnormalities
Corneal Ulcers
What is the cornea?
The cornea is a transparent layer at the front of the eye, and together with the lens focuses light on to the visual part of the eye. It has five delicate layers: the epithelium (outermost layer), Bowman’s membrane, the stroma (thick middle layer), Decemet’s membrane and the corneal endothelium (innermost layer).
A corneal ulcer is where injury or infection has caused a loss of one or more layers of the cornea. Corneal ulcers can be incredibly painful and if left untreated can result in loss of vision or loss of the eye itself.
Symptoms
- Blinking or squinting
- Redness
- Discharge from the eye
- White or blue film over eye
- Swelling around the eye
- Loss of vision
- Loss of appetite
- Pawing at the eye
- Lethargy
- Depression
Causes
- Trauma – e.g. from rubbing the eye
- Laceration or scratch to the cornea
- Dry Eye (keratoconjunctivitis sicca)
- Foreign body – e.g. grass seed
- Eyelid problems such as oversized eyelids, entropian or extra eyelashes
- Chemical burn – e.g. irritation from shampoo
- Bacterial or viral infection
Diagnosis
Your veterinarian will perform an eye examination and gather any relevant history that can help determine the cause. During the eye examination your vet will need to place fluoroscein dye into the affected eye. This dye glows green under a UV light which is best seen in a dark room. If there is a scratch or ulcer present the fluoroscein stain will adhere to that area and your vet will easily be able to identify an injury. This examination is not painful for your pet.
Treatment
- Topical antibiotics and lubricants (eye cream)
- Pain relief (e.g. non-steroidal anti-inflammatory medication)
- Oral antibiotics or anti-viral medications
- Surgery may be required to debride the ulcer, and in some cases temporary eyelid closure will protect the eye until the ulcer has healed
- Eye removal for end-stage ulcers (e.g. ruptured globe)
Serious and complicated cases may require referral to a specialist veterinary ophthalmologist.
If you suspect your pet may have a corneal ulcer be sure to contact your veterinarian ASAP to make an appointment. As already mentioned, corneal ulcers can be incredibly painful and have the potential to leave your pet blind.
Dry Eye – Keratoconjunctivitis Sicca
What is it?
Keratoconjunctivitis Sicca, alternatively known as dry eye, is caused by a deficiency of tear production in the eye. This leads to inflammation and severe drying of the cornea and conjunctiva of the eye. It is more common to see this condition in dogs than it is in cats.
Causes
There are several causes of dry eye, some include, congenital defects, immune-mediated disease, long-term inflammation, inadequate amount of lubrication to the eye when under a general anaesthetic and breed related-predispositions.
Symptoms
- Excessive blinking
- Swollen conjunctiva (looks like a red eye)
- Prominent 3rd eyelid
- Pigmentation and ulceration
- Eyes are surrounded by a thick yellow or white discharge
- Eyes are painful
- Loss of vision
Diagnosis
Your veterinarian will perform a test that measures tear production using a Schirmer tear test strip. The strip is placed at the edge of the eye for a minute allowing for tears to flow up the strip. The amount of wetness on the strip will indicate a measurement of tear production and this is compared to normal levels. If tear production is below normal levels, dry eye may be diagnosed.
What happens if dry eye is left untreated?
- Chronic eye infections
- Repeated irritation of cornea
- Severe scarring
- Corneal ulceration
- Blindness
Treatment
Treating dry eye requires topical medications that stimulate tear production. In some cases where the eye/s are infected, antibiotics and anti-inflammatory medications may also be prescribed.
Cherry Eye
What is it?
Cherry eye, medically known as nictitans glands prolapse, is the prolapse of the gland in the third eyelid. This gland assists in tear production and under normal conditions is not visible. When the gland is exposed it begins to swell and because of its appearance (looks like a little cherry) it’s known as cherry eye.
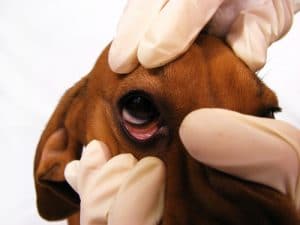
What is the cause?
Unfortunately the cause of cherry eye is not exactly known but it has been suspected that a weakness of the tissues around the gland may contribute to gland prolapse. It has also been thought that the condition is inherited and is more common in particular breeds.
Symptoms
Once the gland has been exposed it can cause irritation and encourage scratching of the eye. This poses a risk to further damage, which leads to swelling, redness and mucous discharge.
Treatment
The gland must be repositioned surgically to minimise the risk of further injury. Medications are rarely effective. Even though the inflammation and pain can be reduced the gland is still prolapsed.
You may also like
Brachycephalic Syndrome
Brachycephalic Obstructive Airway Syndrome (BOAS) affects flat-faced (brachycephalic) dog breeds, such as French Bulldogs, English Bulldogs, Pugs and Boston Terriers.
Laparoscopic Desexing
Laparoscopic desexing offers an alternative method of desexing female dogs and cats from the traditional ovariohysterectomy. It is increasing in popularity amongst both veterinarians and pet owners as it can offer a number of significant benefits.
Laparoscopic Assisted Gastropexy in Dogs
What is GDV? GDV (gastric dilatation and volvulus) is a very sudden and serious condition seen in dogs where, due to range of factors, the stomach first dilates (bloats), and subsequently rotates (twists) on itself. This leads to the entrapment of fluid and gas in the...



